Fibromyalgia
Fibromyalgia is a chronic syndrome characterised by the presence of widespread chronic pain. In most cases it is accompanied by other symptoms:
- Sleep disturbances (insomnia, poor sleep, etc.).
- Cognitive difficulties such as memory problems, attention problems or lack of concentration.
- Somatic symptoms such as headache, irritable bowel syndrome, vertigo or morning stiffness, among others.
- Emotional disorders, mainly depression or anxiety.
The variability of fibromyalgia symptoms explains the impact of this syndrome on patients’ quality of life, as it interferes with their social, work and emotional life. Fibromyalgia is more common in women than in men and mainly starts between the ages of 20 and 50. The disease is diagnosed clinically and there are no complementary tests to indicate that someone is suffering from the disease, but we do have to rule out other pathologies that can produce similar symptoms and that can benefit from specific treatments.
- Treating fibromyalgia
-
The cause of fibromyalgia is unknown and we currently have no treatments that we can define as offering a cure. That said, there is increasing consensus among the medical community that central sensitisation phenomena play a key role in the formation, worsening and persistence of pain. In other words, the central nervous system in fibromyalgia patients processes pain poorly.
Our efforts should focus on controlling the symptoms as far as possible in order to improve the person’s quality of life and increase their activity and participation. Occasionally, patients enter a vicious cycle of suffering with a response from their threat/flight system that leads to them overinterpreting their symptoms and acquiring potentially negative pain avoidance behaviours. Some of the main acquired behaviours are an increase in the consumption of analgesics and anti-inflammatory drugs (most of which are ineffective), giving up physical activity, or the appearance of symptoms like anxiety. All of these situations can help increase or perpetuate the pain.
Cognitive rehabilitation with Guttmann, NeuroPersonalTrainer® is neuropsychological rehabilitation treatment, which is an active process that helps the patient to optimise the recovery of higher functions (attention, perception, memory, executive functions, calculation...) to better understand the alterations presented and to develop strategies to compensate f

The Psychological treatment with Cognitive behavioural therapy brings together two types of therapeutic treatments, because although behavioural therapies are successful in the treatment of some pathologies, other aspects involved in the way in which people respond to different situations have to be taken into account.

This personalised training and improved functionality programme is aimed at optimising and maintaining functional capabilities, as well as preventing complications associated with disability issues.

Neuropsychological rehabilitation or neuropsychological treatment is an active process that helps patients and their families to better understand the difficulties they present, develop strategies that optimize their higher functions, compensate for neuropsychological disorders and optimize higher functions.

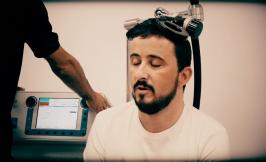
This programme of treatment of neuropathic pain through transcranial stimulation and virtual reality is designed for patients who have suffered a neurological injury and present neuropathic pain after their rehabilitation process is finished, or people in a chronic phase who want to relieve their pain

Guttmann Barcelona has launched its treatment programme for fibromyalgia and pain with group sessions, as the social aspects associated with group therapy provide additional benefits to those of the treatment itself, due to the positive impact that spending time with other people has on our

Guttmann Barcelona offers a treatment programme of physiotherapy and gait rehabilitation in a group, with sessions based on shared rehabilitation goals, with activities being planned around these goals in both the rehabilitation room and the swimming pool.
Et pot interessar
 Monday, 30 March, 2020
The Institut Guttmann will treat Alzheimer's, depression and pain in the new building
Monday, 30 March, 2020
The Institut Guttmann will treat Alzheimer's, depression and pain in the new building
The new Guttmann Brain Health Institute (GBHI), located in the new building in Barcelona, will offer specialized programs for the treatment...